Diabetes is a dangerous condition under which to live — especially if you aren’t properly caring for yourself. Those who live with diabetes must be careful to eat right and get enough exercise. Even though new medical advancements provide a much better outlook, they don’t mean anything if you can’t manage the symptoms. These are some of the worst long-term adverse health effects of mismanaged diabetes.
Without proper self-care, diabetics will likely sustain increasingly severe damage to blood vessels (most common in the legs, heart, and brain). Damage to smaller blood vessels is common in feet, kidneys, and eyes. Nerve damage is common. But long-term health effects will damage one system after another. You will notice digestive troubles, skin trouble, performance issues, and a weakened immune system.
Because those with diabetes often have increased cholesterol, it’s important to reduce consumption of meat and dairy products. Those who suffer from diabetes are also subject to increased blood pressure. These issues can lead to cardiovascular disease. Do you have a family history of diabetes, cardiovascular disease, or both? You’re even more at risk.
Diabetics are subject to various eye diseases, including retinopathy, macular oedema, cataracts, and glaucoma. These diseases can result in permanent damage and loss of vision, and sometimes present with few or no symptoms. If you suspect that your vision is impaired due to diabetes complications, seek medical attention immediately!
Diabetics are also subject to kidney disease because of damage to small blood vessels. This is another complication that might present with few or no symptoms at first.
Severe nerve damage might also occur. This is due to high blood glucose, alcoholism, and vitamin B12 deficiencies, the last of which might result from diabetes medications. Nerve damage often presents in feet, legs, hands, arms, chest, and stomach. Damage to appendages is one of the reasons why diabetics are at risk of infection or amputation.
The feet are especially prone to nerve damage when blood supply is reduced or restricted. More serious complications often arise because the body’s natural healing processes are slowed dramatically while the risk of infection is increased. Those who suffer from diabetes might note numbness or reduced feeling in the feet. Ulcers are common.
The structural purpose of skin is to reduce the probability of infection. Diabetes often results in excessively dry skin — and that means an increased opportunity for infection everywhere.
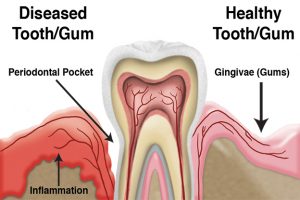
Tooth decay and gum infections also result from restricted blood flow.
Because other health issues can result in increased levels of stress, diabetics are more susceptible to mental health problems. Anxiety and depression can also result in fluctuations in glucose levels, making the disease even more dangerous.


 Along with a long list of other complications,
Along with a long list of other complications,